Adenoid Hypertrophy in Children: Airway Obstruction, Craniofacial Development, and Surgical Indications
Adenoid hypertrophy in children involves nasopharyngeal lymphoid tissue growing large enough to block airflow in the nasal passages. In addition to causing chronic nasal congestion and mouth breathing, adenoid hypertrophy interferes with normal breathing patterns and influences facial development. Studies indicate that children with adenoid hypertrophy have less nasopharyngeal volume and higher airway resistance, which often leads to low oxygen levels, poor sleep quality, and various pediatric sinus issues.
Adenoid Facies
Adenoid hypertrophy is closely linked to changes in facial structure, a condition called adenoid facies. Children with adenoid facies usually have longer faces, narrow dental arches, and high palates. Breathing through the mouth over time can cause the jaw to recede, leading to uneven facial features that can affect how the tongue rests in the mouth. These signs also correlate with chronic pediatric sinus issues such as allergies and sinusitis.
Craniofacial and Dental Changes Associated with Chronic Obstruction
Adenoids that enlarge abnormally narrow the nasopharyngeal space and hinder airflow into the oropharynx. Swallowing and speech quality are also impacted since nasal airflow development promotes the ability to articulate words clearly. Reduced airflow, mouth breathing, and dry mouth also increase the risk of sinus and respiratory infection. Additionally, the blockage raises resistance in the upper airway, making children more susceptible to sleep-related breathing issues.
Diagnostic Evaluation and Therapeutic Interventions
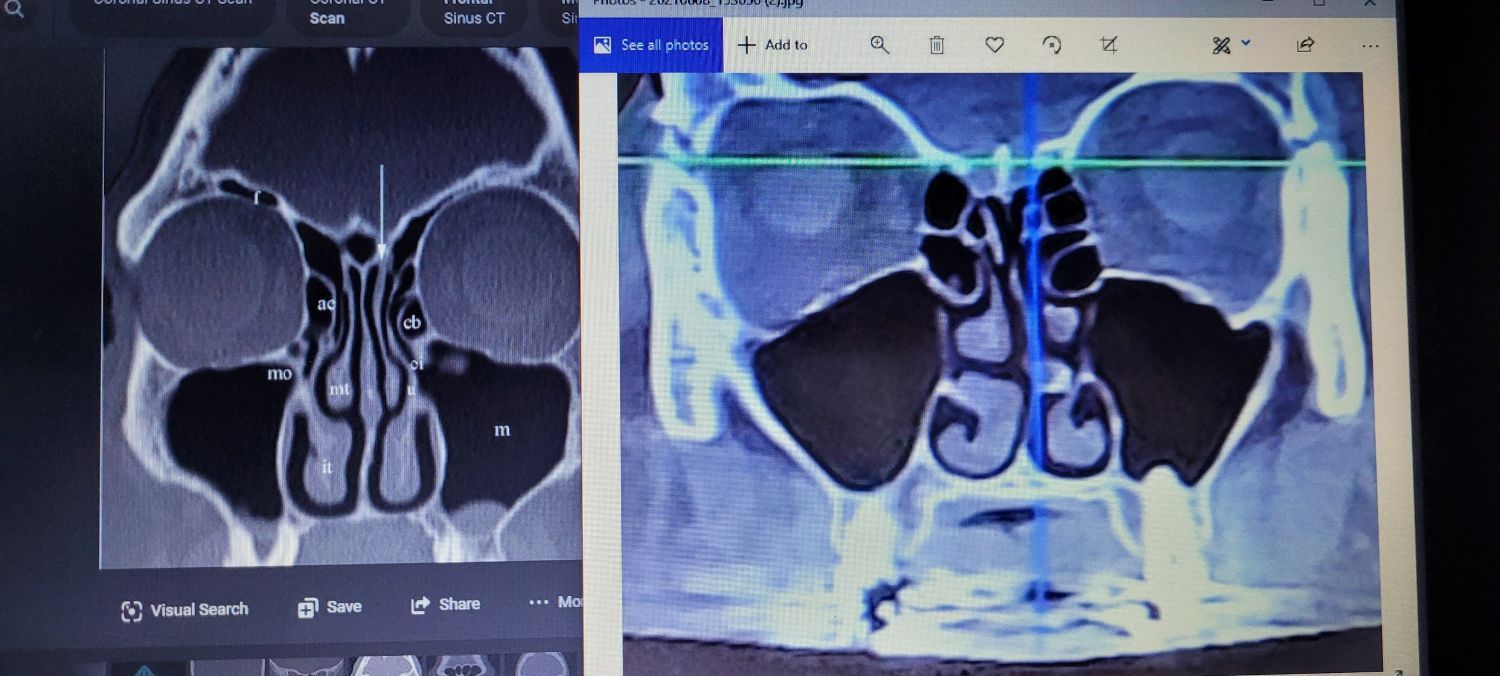
Addressing adenoid hypertrophy starts with a thorough assessment using imaging, nasal endoscopy, or lateral neck X-rays to determine how severe the blockage is. Mild cases may improve with medical treatments like intranasal corticosteroids, anti-inflammatory medications, and allergy management. However, enlarged adenoids that do not respond to medications often require surgical removal through an adenoidectomy.
When is adenoidectomy indicated in children?
Adenoidectomy is performed when adenoid hypertrophy causes persistent nasal obstruction, breathing problems during sleep, pediatric sinus issues, or recurrent otitis media.
Can intranasal corticosteroids effectively reduce adenoid size?
Short courses of intranasal corticosteroids can temporarily shrink adenoid tissue and relieve nasal blockage but are not considered a long‑term alternative to an adenoidectomy.
Are there any preventive measures parents can take to reduce the risk or severity of adenoid hypertrophy in children?
Practicing good hygiene, minimizing exposure to allergens and irritants, and seeking early treatment of infections may help reduce the risk of adenoid hypertrophy in children.
Join the Snot Force Alliance and connect with leading specialists dedicated to advancing sinus, allergy, and airway care through collaboration and innovation. Become a Protector of the Unified Airway today and help us improve patient outcomes while learning about the newest research and treatments.